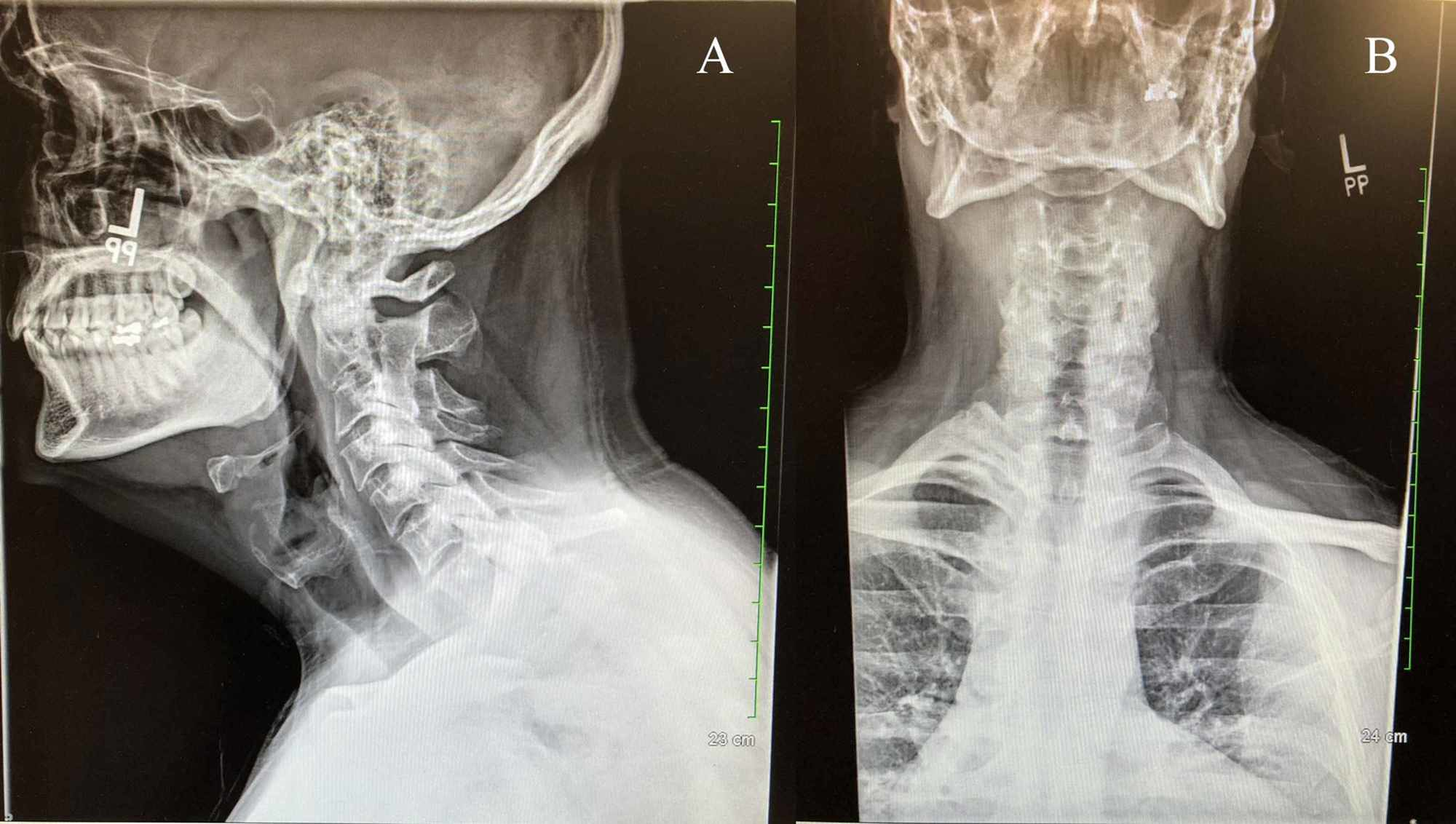
Failed back surgery syndrome (FBSS) is definedĪs failure to relieve lower back pain symptoms following surgery. Is a common belief that immobilization and/or removal of the painful Instrumentation are the main surgical procedures performed in the U.S. Decompression and occasional arthrodesis with frequent Pain is the third most common indication for surgical procedures in the Pharmacotherapy typically resolve such pain. Noninvasive methods of treatment such as physical therapy and Fortunately, in mostĬases, the underlying pathology is benign and the pain is self-limited. Population experience low-back pain each year. It is the second mostįrequent reason for visits to a physician and ranks fifth as the reasonįor hospital admission. Younger than 45 years in the United States. Tehranzadeh isĬhief of Radiology at Long Beach VA and Professor Emeritus and ViceĬhair of Radiology, Department of Radiological Sciences, University ofĬalifornia, Irvine Medical Center, Orange, CA.īack pain is the most common cause of limited activity in people Hayeri is a former Research Fellow, Division of MSK Imaging at University of California, Irvine Medical Center, Orange, CA, and Dr. AOSpine Thoracolumbar Spine Injury Classification System: Fracture Description, Neurological Status, and Key Modifiers. Discrimination of Metastatic from Acute Osteoporotic Compression Spinal Fractures with MR Imaging1. Spinal compression fractures in osteoporotic women: patterns and relationship to hyperkyphosis. De Smet AA, Robinson RG, Johnson BE et-al. Osteoporotic vertebral compression fractures and vertebral augmentation. The treatment of symptomatic osteoporotic spinal compression fractures. Kyphoplasty: balloon-assisted variant of vertebroplasty Medications: bisphosphonates for osteoporosis Retropulsion (not posterior bulging) of the posterosuperior cortex of the vertebral body 
Low signal intensity band on T1WI and T2WI indicating a fracture line Preserved normal fatty bone marrow T1WI signal The following features favor the diagnosis of a benign compression fracture: Osteoporotic vs pathologicalĭiscriminating between acute osteoporotic fracture and pathological fracture is sometimes challenging. In uncertain cases, MRI signs of edema (acute) and the presence of radiotracer uptake on bone scintigraphy (acute) help decide the age of the fracture. 
On conventional imaging, acute fracture signs include cortical breaking or impaction of trabeculae in the absence of these signs fractures are chronic. Acute vs chronicĬhronicity of the fracture indicates its temporal relationship with symptoms and hence is an important determination. When in doubt, it is recommended that additional views or studies be advised for confirmation. The vertebral fracture should be diagnosed when there is a loss of height in the anterior, middle, or posterior dimension of the vertebral body that exceeds 20%. This defines the role of the radiologist in making an accurate diagnosis. 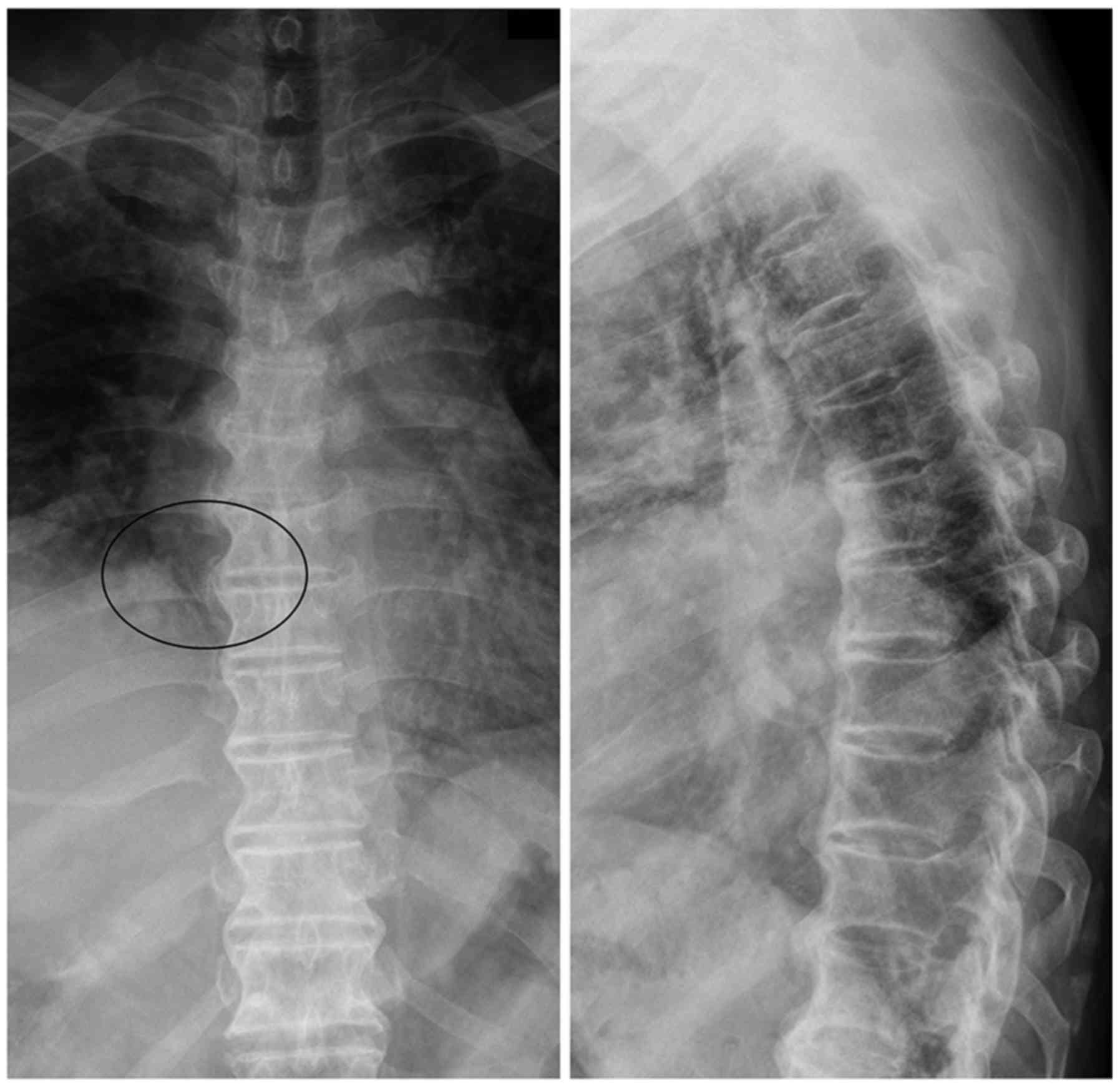
Vertebral fractures require treatment when they are symptomatic, i.e. with pain and loss of mobility. Osteoporotic spine fractures can be graded with the Genant classification of vertebral fractures based on vertebral height loss as: See: AO spine classification of thoracolumbar injuries. Pincer or split fracture: involvement of both endplates but not the posterior wallīurst fracture: involvement of one endplate (incomplete) or both endplates (complete) and the posterior wall Wedge compression fracture: involvement of one endplate but not the posterior wall PathologyĬompression fractures can result from osteoporosis, trauma or represent a pathological fracture secondary to another process (e.g. Vertebral fractures present with pain and loss of mobility. However, they are largely unreported and are probably more common radiographically (present up to 14% of women older than 60 years in one study 1). person-years after 85 years of age in the United States.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
